Coronis Health, Laboratory & Pathology
Laboratory & Pathology
Outsource laboratory billing for hassle-free financial growth and uncover hidden revenue
Industry Insight: Connect to former lab leaders who bring a deep understanding of lab operations for tailored solutions.
Advanced Lab Technology: Leverage AI-powered solutions to increase cash flow and reduce lab workload.
Serving Diverse Labs and Pathology Practices: From molecular diagnostics to hospital outreach labs, we cater to a wide range of specialties.
Hear What Our Clients Have to Say
Read Our Latest Case Studies
Improved Processes, Better Outcomes
Case Studies
Laboratory & Pathology
Coronis Health Helped Increase Revenue by 7% Year-Over-Year
The Lab Team at Health System X was looking to understand and improve billing capability. Coronis Lab offered a unique opportunity to provide industry expertise and billing support.
Coronis Health Becomes Part of Our Client’s Practice Fabric for All to Benefit
With care and special attention, Coronis was able to up the practice’s revenue while retaining a the local billing presence the client desired.

For Labs. For Pathologists. Coronis Health Makes the Difference.
Coronis Health Laboratory & Pathology is the catalyst for improved financial and operational outcomes, allowing you to focus on providing exceptional testing and diagnostic services.
With a team of experienced lab and pathology professionals, we can help your practice:
- Expand your testing services
- Uncover hidden revenue streams
- Strengthen your bottom line
Experience the real impact that Coronis Health can bring to your lab and pathology practice.
-
Seasoned Lab Professionals Joining Forces
With a team of former lab professionals, Coronis has a deep understanding of RCM for various types of labs, enabling labs to shift their focus back to their core responsibilities.
-
Technology That Captures Every Last Dollar
Advanced artificial intelligence meets superior A/R processes to improve cash flow and drive cash into clients’ pockets with Ai4AR™ and RCM Clarity™.
-
A Client-Centric Approach for Building Long-Lasting Partnerships
We build strategies with our clients through transparent communication and easy access, supported by honest reporting, and our leadership and team members are readily available to clients via email or phone.
-
Data-Driven Decisions to Drive Meaningful Results
Our team implements proprietary analytics from the beginning that identify and close gaps in the RCM process to help boost revenue.
Our Capabilities
Laboratory Analytics
Analytics shouldn't stop you from efficiently running your lab. Let us take care of the analytics, while you leverage the data to make informed decisions about your day-to-day operations. As laboratories continue to grapple with high-volume, low-dollar testing, high staff turnover, and evolving COVID-19 guidance, it’s now more important than ever to implement data analytics […]
Automation Tools & Ai4AR™
Human error is one of the leading causes of claim denials in medical billing and revenue cycle management (RCM). Data entry, researching claim information, and other manual processes are time-consuming and vulnerable to mistakes. While these errors may seem minor, they can slow your reimbursement rate and diminish your revenue. With 35+ years of experience, […]
System Integration
Coronis Health integrates the technologies and systems we've partnered with to provide the best service possible to our pathology and lab clients.
Focused Accounts Receivable Process
Coronis Health is at the forefront of AI for AR, using Artificial Intelligence to completely revolutionize how we collect. Not only does it save money, but it will save time and learn as we go.
Consulting
Coronis Health consulting services ranging from Revenue Cycle Assessment to Quality/Productivity Design.
Proprietary Technology
Just as it is important to have a highly experienced team of revenue cycle management professionals on your side, it is equally important to arm those professionals with industry-leading tools to make laboratory RCM more efficient and effective. Not all laboratory billing companies have the same tools at their disposal to help clinical laboratories maximize […]
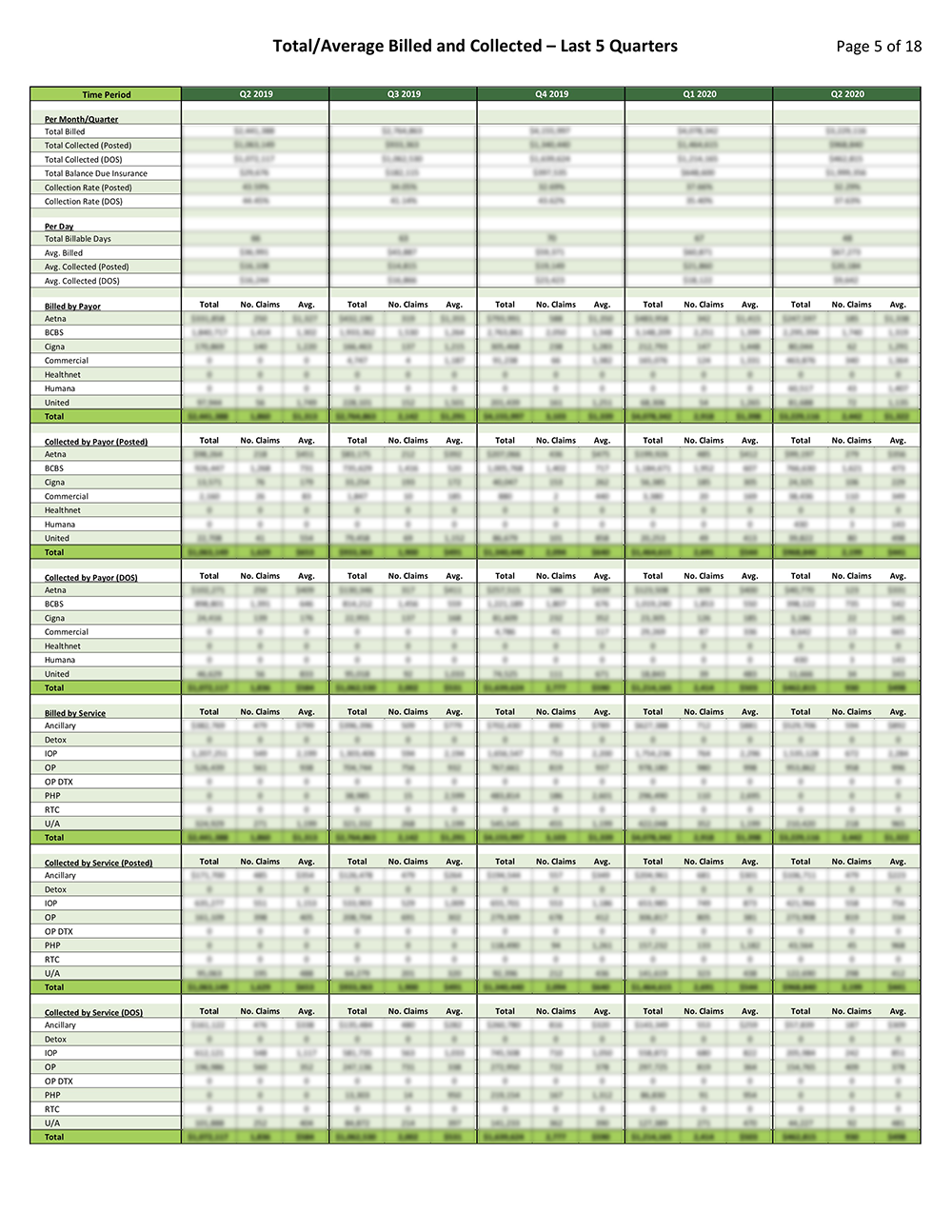
Account Management and Financial Reporting
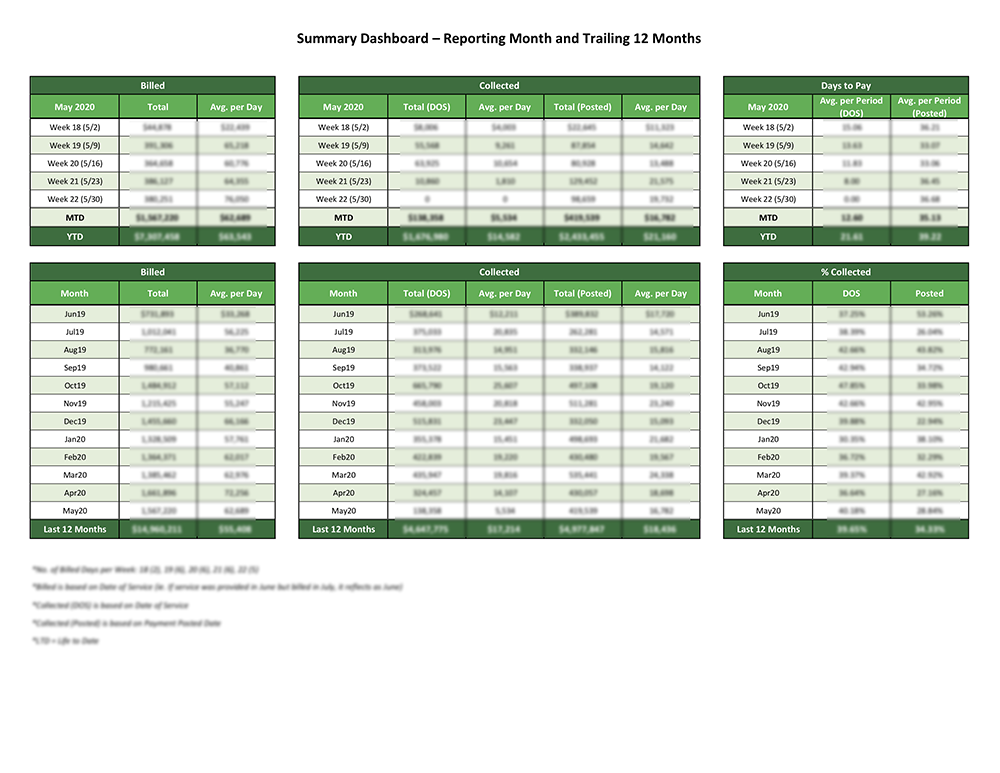
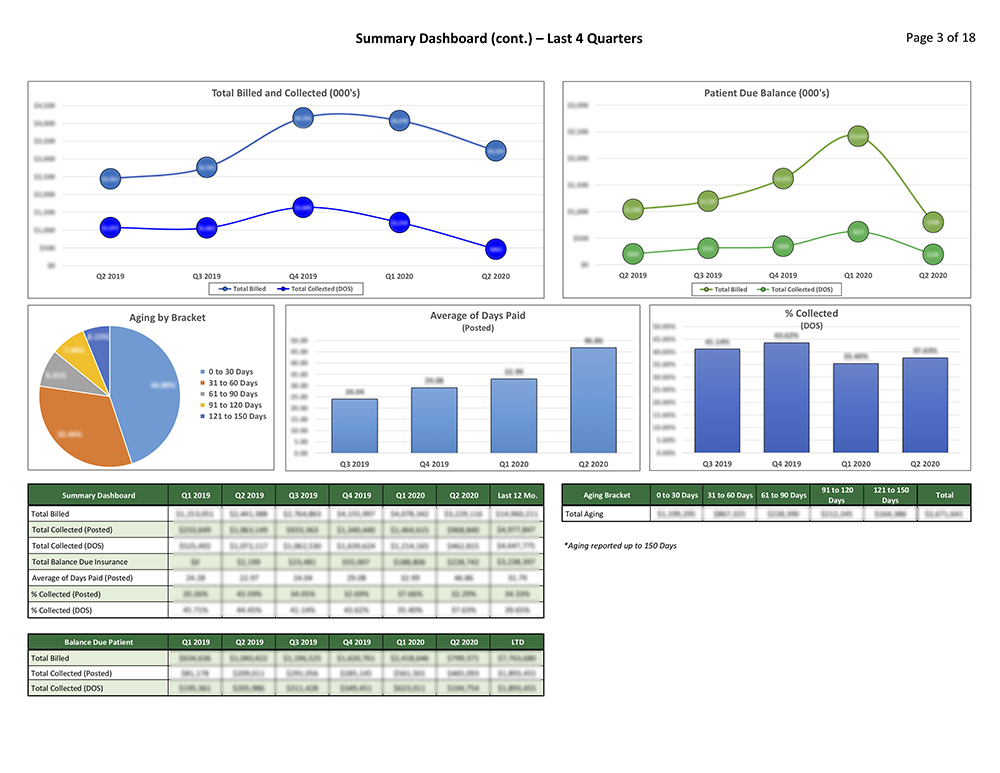
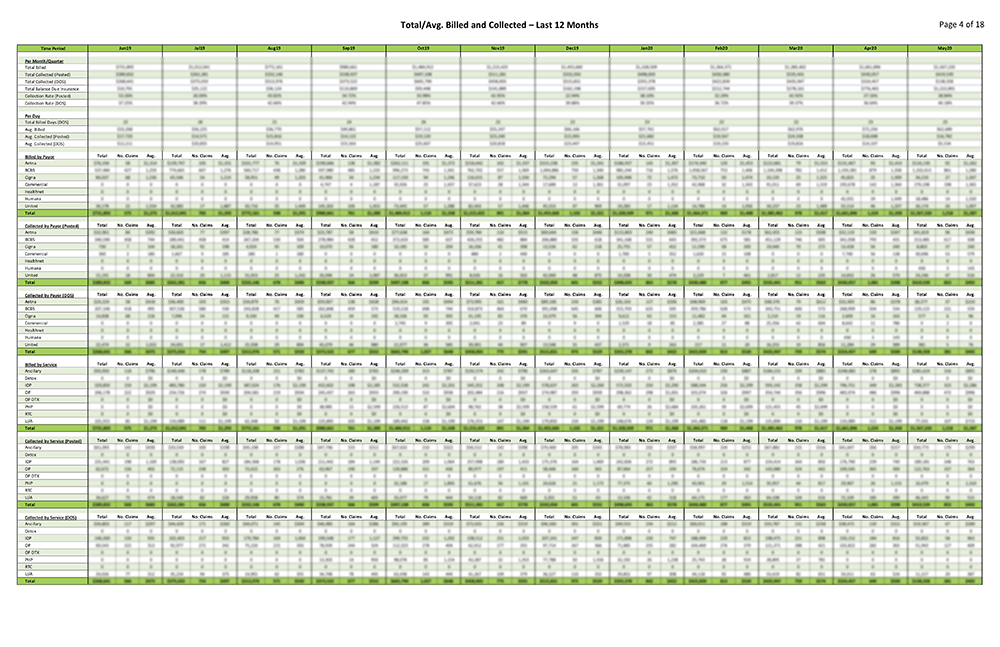
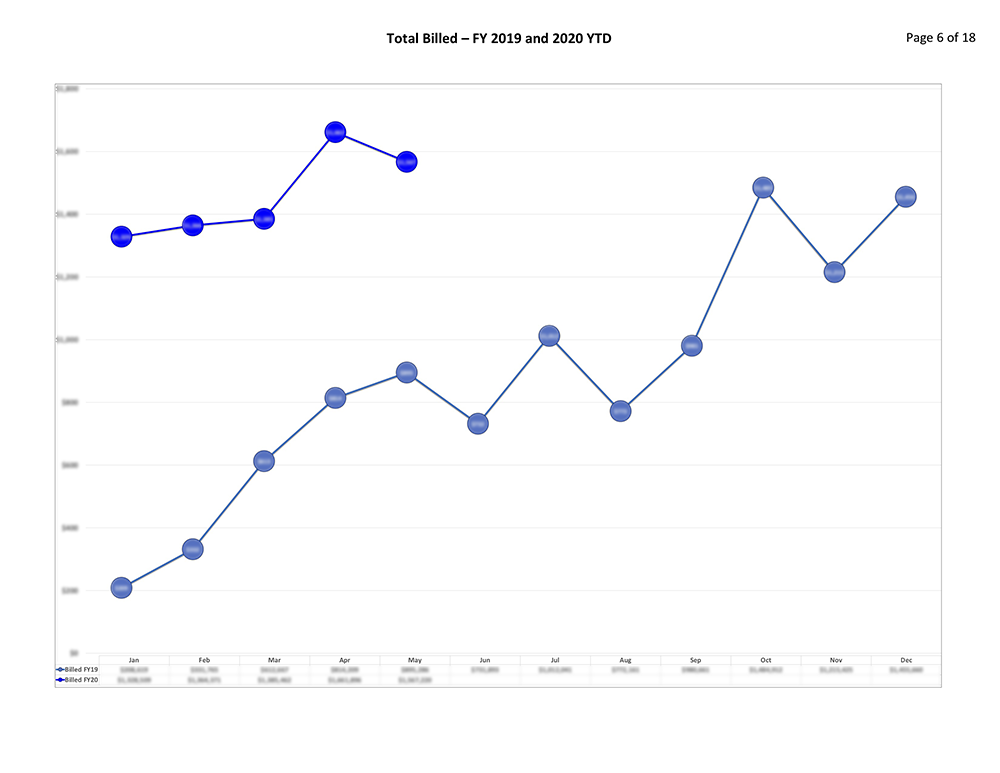
Coronis Health provides a detailed “Report Card” that tells you everything you need about your business in a quickly digestible format. We don’t just tell you the numbers, we tell you why the numbers matter.
Testimonials
“Looking for the right company for billing and reporting? This is truly the one as they provide much more, seamlessly and accurately. Want to think you are the only client, then look no further. They are always on top of things that will be important to you as a Practice Manager, Lab Manager or Owner.”
Multi-state Pathology Group
Based In California
“Coronis is more than a vendor to our laboratory; they are a partner to our lab that is a crucial component to our success. Billing can be a problematic area of service for the lab, but with Coronis Health as our trusted partner, we are able to focus on the growth of our core business and serving our patients and community.”
David Nichols
President, Pacific Diagnostic Laboratories
Santa Barbara, CA
“Coronis Health has been a valued and trusted partner in providing billing services to Sentara Reference Laboratory for seven years. Their expertise and performance, as well as their ability to customize solutions and applications to our situation, has played an important role in the growth and success of our lab outreach program.”
Andrew P. Weddle CPA
Vice-President Finance, Sentara Healthcare
Norfolk, VA
“Coronis Health has been a great partner in supporting the development of Carilion Labs and strengthening our financial performance through effective revenue cycle services, and, as importantly, through providing enhanced business intelligence functionality and insight.”
Bud Thompson
Senior Vice President, Carilion Labs
Roanoke, VA
“We have used this company many years as our billing service. Coronis Health has been an exceptional partner to work with. I would highly recommend them for any and all medical billing needs.”
Ginger Helton
Practice Manager, Pathology Associates
“Coronis is doing a great job for our pathology practice. I highly recommend them.”
“Coronis Health does an excellent job with our billing and collections! We appreciate the professionalism, consistency and dependability of the Coronis Health personnel and would highly recommend this company to other medical groups.”
“I have been working with PDM/Coronis Health for about 9 years now as our billing services agency and I have never been let down by its performance. They know the medical billing business very well. Knowledgeable, responsive, and true professionals.”
“I am continually grateful for PDM’s integrity in ensuring accurate services.
PDM understands a client providers’ financial success is a direct reflection of PDM’s ability to accurately capture charges and post payments in a timely manner!”
“PDM REACTS to the market. They stay current and ontop of any regulatory issues. They are sensitive andaim to improve the economics of your operation. Theyhelp with the administrative issues of billing and theimpact their collections has on your business. Theyprovide excellent customer service and follow through.They add value to your operation by providing themost current technology with information systemsand AI. This approach keeps Coronis PDM at the front of Pathology billing and collections!”
Integrations and Partnerships
Team

Tony Mira
Interim Chief Executive Officer

Fred Fazio
Chief Financial Officer

Doug Marcey
Senior Vice President of Technology

Kai Williams
Chief Human Resources Officer

Neda Ryan
General Counsel

Markus Muhlhauser
Senior Vice President
More About Coronis Health
Sophisticated Lab and Pathology practices know that their most important financial asset is their billed services and accounts receivable. This asset needs to be safeguarded, well-organized, tightly managed, and carefully maintained by a professional team possessing a perfectionist approach to execution, accuracy, follow-up, and timeliness.
Many laboratories today simply cannot devote the same resources and attention to billing which the Coronis Health Lab is able to provide its clients. We understand the challenges of today’s increasingly complex and ever-changing lab billing environment. Our lab billing team employs many former lab directors and pathologists, giving us the advantage of industry-leading knowledge and experience. Focusing exclusively on lab billing enables the Coronis Health Lab to make billing an outstanding core competency for our clients.
Your billing department needs to maximize employee productivity, collections, and provide the lab with the necessary business intelligence to make quick and confident strategic decisions. The Coronis Health Lab’s sole focus is to ensure your lab is a pioneer in all of these key success factors. In a world of changing regulations and reimbursement trends, Coronis will ensure that your lab retains a best-in-class billing capability.